Anthrax is a potentially fatal infectious disease caused by a gram-positive bacterium that can affect both animals and humans. In developed sections of the world, particularly Europe, the disease is extremely rare, but isolated cases have been reported in the Mediterranean countries, Hungary, and Romania in recent years.
Anthrax is a biological weapon that has been utilized by several countries in the past. The most recent serious bioterrorism incident happened in 2001, when anthrax spores were delivered via the US Postal Service to US citizens. During that time, 22 persons were sick after receiving or opening tainted letters, with five of them dying.
What causes anthrax?
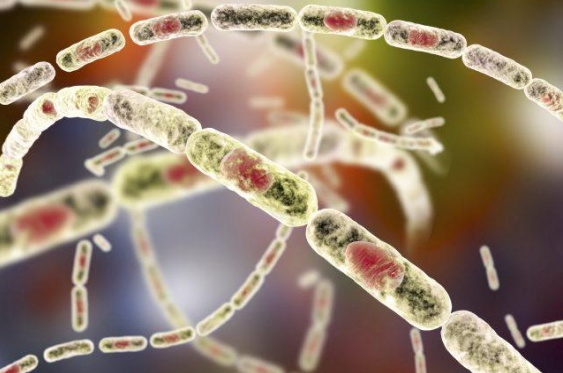
Bacillus anthracis, which can be found in soil and causes disease in herbivores like cattle, sheep, and goats, causes anthrax. The bacterium comes in two types: slow and vegetative.
Spores can only form outside of the body, most commonly when infected blood from an animal exits the body and comes into touch with air. Spores are incredibly stable and resistant to external effects, allowing them to exist for years.
The second type is the vegetative form, which occurs when spores enter the organism (animal or human). Because spores “sense” the difference between dirt (which has limited nutrients) and live beings, they convert from spores to vegetative form (where nutrients are abundant).
Humans are most typically infected by direct contact with an infected animal or its products, whereas animals infect spores by grazing and therefore become infected (meat, animal hair, etc.).
Who is at a higher risk of becoming infected with anthrax?
Natural exposure to the bacterium’s spores is highly unlikely in the vast majority of the population. Unfortunately, due to a larger possibility of being exposed to the causative agent, a certain group of people is at a higher risk of infection.
This group includes:
- Veterinarians;
- Persons working with animals or animal products (skin, animal hair, meat);
- Livestock;
- People working in an anthrax lab.
How is anthrax transmitted to humans?
The natural occurrence of the disease in humans is through contact with infected animals or animal products (eg meat, skin, animal hair).
There are 3 ways to get spores into the body:
- Inhalation of spores;
- Penetration of spores through microdermabrasion of the skin;
- Ingestion of spores (oral intake).
Depending on how the spores entered, we distinguish 3 clinical forms of the disease:
- Inhalation anthrax
- Cutaneous anthrax
- Gastrointestinal anthrax
Inhalation anthrax does not spread from person to person, meaning that a person afflicted with it cannot infect another person.
In the event of cutaneous anthrax, there is a very low risk of infection from person to person, which could occur if someone came into direct touch with the patient’s skin wound.
What are the indications and symptoms?
The clinical form determines the disease’s symptoms and manifestations.
- Anthrax inhalation It is estimated that 10,000 spores are required for breathed anthrax to grow. The disease’s early symptoms are non-specific and mirror the clinical picture of a viral syndrome: fever, weakness, malaise, dry cough, which increases after a few days, followed by chest pain and discomfort, coughing up blood, choking, and hunger. If therapy is not started right away, further respiratory and gastrointestinal symptoms and indications develop quickly, and most cases are fatal within 24 to 48 hours.
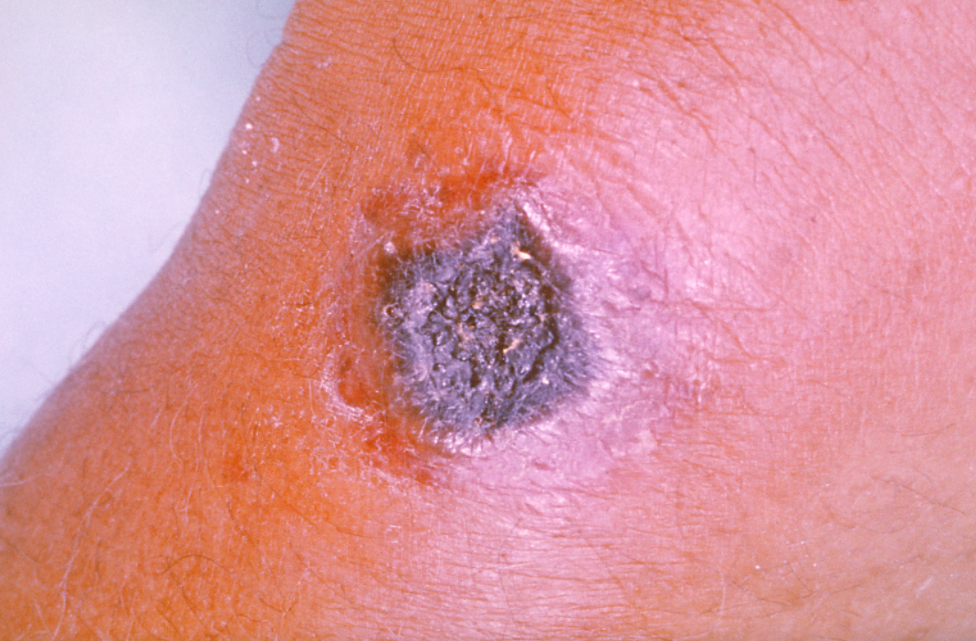
- Cutaneous anthrax is a type of anthrax that affects the skin. Cutaneous anthrax arises when spores penetrate the skin through a small opening (microwave). One week after exposure, symptoms appeared. Any portion of the body might be affected, although the most common areas are the face, neck, shoulders, and arms. Itching and redness emerge at the infected area of the skin, followed by swelling that develops into a painless ulcer with a charcoal black appearance (black patch). Anthrax is derived from the Greek word anthrax, which signifies coal.
Because antibiotics are available, the cutaneous type of anthrax is only lethal in about 20% of cases.
- Anthrax in the gastrointestinal tract. When spores are taken orally, as as when eating contaminated meat, this type develops.
Symptoms and signs include:
- Nausea;
- Vomiting (more advanced blood vomiting);
- Fever;
- Decreased appetite;
- Diarrhea;
- Severe abdominal pain.
In some cases, there may be difficulty swallowing and swelling of the lymph nodes in the neck.
If this form is not treated in time, it ends in death in 25-60% of patients.
How is anthrax diagnosed?
Additional tests, such as laboratory, microbiological analysis, and radiographic diagnostic, are required to make a definitive diagnosis, in addition to a good history and clinical picture.
Treatment and prevention
Anthrax can be successfully treated if detected early and treated promptly. People who have had reliable or suspected contact with the bacteria should be treated with broad-spectrum antibiotics. Antibiotic therapy should be avoided if the person has been known to have been exposed to the spores.
There is an anthrax vaccination available in some countries, but it is not for the general public; instead, it is for persons who are at risk of infection.
Important! A timely and precise diagnosis, as well as the prompt start of antibiotic therapy, are critical to surviving anthrax infection. If you have any of the symptoms listed above and fear you’ve been exposed to anthrax spores, see your doctor right once.